Race and Health
Arthur Holloway, American Renaissance, May 1996
On average, blacks are less healthy than whites and die sooner. They are more likely to die in infancy, get serious diseases, or die from accidents and murder. All of this is usually attributed to “racism” — either to direct harm caused by a prejudiced medical establishment or to the effects of the poverty and ignorance that are said to flow from racism.
In the medical literature, the higher rate of death for blacks — from virtually all causes — is called “excess deaths.” Every year, there are approximately 80,000 such “excess deaths,” or deaths that would not have occurred if blacks were as healthy and lived as long as whites. Calculations of this kind are often presented as measures of how racist American society is and how much blacks suffer on account of living in it.
Implicit in this measure, however, are three assumptions. One is that whites are the healthiest, most long-lived group, and are therefore the standard by which all others should be judged. Another is that all races have the same genetic potential for good health and long life. The third is that all races take equally good care of their health.
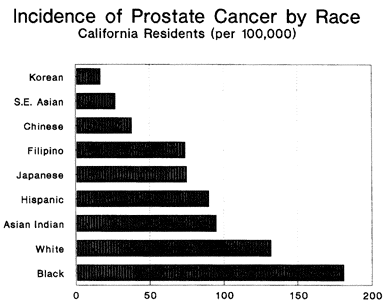
All three assumptions are false. To begin with, whites are by no means the healthiest Americans. Asians and Pacific Islanders (of which only five percent are Pacific Islanders) outlive whites by an average of seven years — exactly as long as whites outlive blacks. There are therefore 480,000 “excess deaths” among whites as compared to Asians, though no one seems to notice or care.
Secondly, science is steadily demolishing the view that races are genetically equivalent. For example, it is now well established that endemic malaria in West Africa resulted in genetic selection for blood abnormalities (technically known as hemoglobinopathies) that protect against malaria but can have dangerous side effects. Only blacks, therefore, get sickle cell disease and certain forms of thalassemia, which have indisputably genetic origins. It likewise appears that cancers behave differently, and more dangerously, in blacks than in whites for reasons that also appear to be genetic.
Finally, people of different races have different habits that affect their health. The U.S. Center for Disease Control reports that 38 percent of black women, 22 percent of white women, but only 10 percent of Asian and Pacific Islander women are overweight. The figures for men are blacks, 28 percent; whites, 25 percent; and Asians, 10 percent. The CDC also reports that American Indians and Alaska natives are heavy smokers. Forty-two to 70 percent of Northern Plains Indians and 56 percent of Alaska natives smoke as opposed to a rate of 29 percent for whites.
Nevertheless, in seeking the causes of racial differences in health and longevity, it is very difficult to untangle behavior, genetics, and environment. Some groups, for example, may be genetically predisposed to obesity or may become more easily addicted to nicotine. Smoking and obesity may be “environmental” factors that are mediated by genes.
Also complicating any analysis of causes is the fact that in all racial groups, the rich are healthier and live longer than the poor. Income therefore accounts for part of the health gap between whites and blacks and, because Asians have particularly high incomes, for part of the gap between Asians and whites. However, racial differences persist even when income is held constant; rich blacks die younger than rich whites, who die younger than rich Asians. Nor is income itself independent of genetics. Although wealth certainly buys good medical care, it also reflects traits that are associated with good health and long life: intelligence, discipline, and foresight.
Finally, medical and public health advances affect people of all races. During this century, life expectancy of both blacks and whites has increased by more than 30 years. Since 1915, white infant mortality has dropped from one in ten live births to fewer than one in a hundred. The black rate has dropped from one in six or seven to one in sixty. A black child born today has the life expectancy of a white child born in 1950.
Despite these complexities, there are racial differences in disease patterns that point strongly to biological rather social causes.
Infant Mortality
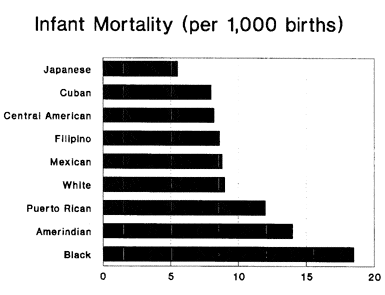
Much is made of the fact that the black infant mortality rate is more than twice the white rate. This is repeatedly cited as proof of “institutional racism,” and the poor medical care granted to blacks. However, there are plenty of racial groups in this country that have lower infant mortality rates than whites (below). The lowest are the Chinese and Japanese, who have higher incomes than whites, but Central Americans and even Mexicans — who have incomes almost as low as blacks — do as well or better than whites.
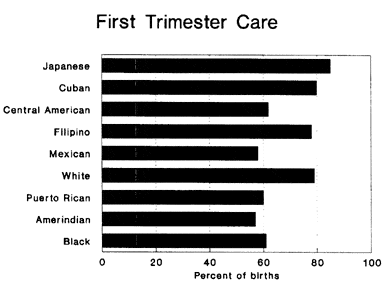
The graph below shows the percentage of mothers of each group who see a doctor during the first three months of pregnancy — the most common indicator of adequate pre-natal care — and the graph after that shows the percentage of different groups that do not have medical insurance. The second and third together show that prenatal care can be as much a matter of initiative as of formal medical coverage. Cubans, for example, are slightly more likely than blacks not to have medical insurance of any kind, but 80 percent of Cuban mothers (20 percent more than black mothers and slightly more than white mothers) manage to get first trimester treatment. In the United States there is medical care for any pregnant woman who wants it.
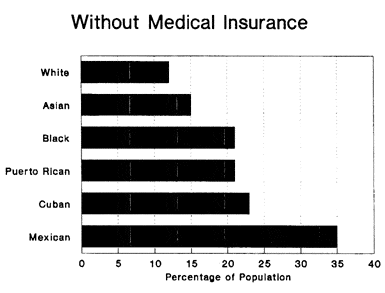
Mexican-Americans should have just about the highest infant mortality rates in America. They are almost as poor as blacks, less likely to finish high school, less likely to have insurance, and less likely to see a doctor during the first three months of pregnancy. They are also more than twice as likely as the rest of the population to give birth outside a hospital (2.5 percent of the time v. less than one percent). Yet, the Mexican-American infant mortality rate is slightly lower than the white rate (8.8 per 1000 births v. 9.0 per 1000 births) and well below the black rate of 18.7.
In terms of income and education, Puerto Ricans are comparable to Mexicans, with the difference that they are more likely to have medical coverage and to see a doctor during the first trimester. Yet their infant mortality rate is one of the worst in the country. Differences as consistent and dramatic as these suggest that races simply differ in their ability to survive the first year of childhood. All races respond to improvements in medicine and public health but inherent traits remain unchanged.
Another interesting indicator of health differentials is the rate at which people die from accidents. Although data for specific causes are available only for blacks and whites, the differences are significant. As a group, blacks are more likely to drown than whites. However, between the ages of one and four the likelihood is reversed because white children are more likely to be near residential swimming pools.

The usual explanation for the high rates at which blacks die in residential fires is that they live in decrepit houses without smoke alarms or fire escapes. However, it is significant that women of both races — who presumably live in the same houses as men — are considerable less likely than men to die in fires. This suggests a difference in temperament which may well exist between the races as well.
High rates among blacks of pedestrian death in auto accidents are not easy to explain in terms of poverty. Finally, it is hard to think of any explanation but greater recklessness for the fact that black men who own guns are five times more likely than white men who own guns to be involved in fatal firearms accidents (not shown on the chart).
Other data are available on accidental deaths from all causes for people of different races in the most accident-prone years: ages 15 to 24. American Indians die from accidents at a rate of about 90 per 100,000 or nearly twice the white rate of 55 per 100,000. Hispanics have a rate almost identical to whites, at 50 per 100,000, while Asians and Pacific Islanders have the lowest rate at about 32 per 100,000.
Hardy Asians
The two below tables show annual death rates per 100,000 population for the diseases from which people most frequently die. Men and women die from many of the same diseases but at different rates, so there is a table for each sex. The figures are adjusted by age, so that comparisons are between equivalent populations. Blacks, Hispanics, and Asians are all relatively young populations. Since mortal diseases usually strike old people, death rates must be adjusted by age so that non-white death rates do not seem artificially low.
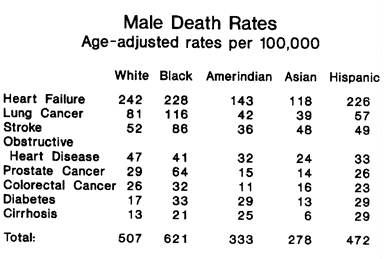
Among men, blacks have the highest death rates for five of the eight diseases. Whites have the highest rate for two of the remaining diseases (both are heart diseases) and have the second highest rates, after blacks, for five diseases. Hispanics have the highest rate of cirrhosis. Asians and Pacific Islanders have the lowest death rates in all but one category — stroke — in which only American Indians have a better record.
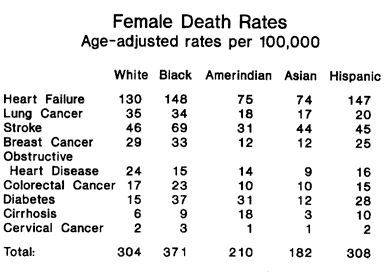
For women, the situation is similar. Blacks lead in six out of nine diseases, and whites lead in two of the remaining three. Whites are second only to blacks in five out of nine diseases. Asians have the lowest rates in seven out of nine diseases and, again, are bettered only by American Indians, who have lower rates of stroke and colorectal cancer. For both sexes, adding up all the causes of death shows that there are far more “excess deaths” of whites by Asian or even American Indian standards then there are “excess deaths” of blacks by white standards. Presumably, this is of no importance.
The figures for Asians mask substantial differences between nationalities. Although Chinese, Japanese, Filipinos, Koreans and subcontinental Indians account for 80 percent of Asian-Americans and generally fit the health and economic patterns for this group, some Asian peoples do not. Poverty rates for Hmong (63 percent), Cambodians (43 percent), and Laotians (35 percent) are much higher than for Chinese, Japanese and Filipinos (6-8 percent), though the first three groups make up only 5.6 percent of the U.S. Asian population.
Southeast Asian men also smoke more than anyone else in America: Vietnamese (60 percent), Cambodians (71 percent), and Laotians (92 percent). Very little is known about disease rates for these subgroups, but they are likely to be much higher than for Asians as a whole. Pacific Islanders, who are “Asians” for statistical purposes, also bring down the average. Hawaiians, who account for 60 percent of the group, have a life expectancy lower than whites, as do Samoans, Guamanians, Tongans, and other islanders.
It makes no medical sense to treat Laotians and Samoans the same as Chinese or Japanese, but that is how the data are gathered. Including islanders and Southeast Asians increases death rates and infant mortality rates for “Asians and Pacific Islanders,” and means that the North Asian health record is even more impressive than this data suggest.
In general, American Indians come closest to Asians in their likelihood of dying from different diseases. This is not surprising, since they are thought to have crossed the land bridge from Asia only 35,000 to 40,000 years ago, and are closely related to North Asians. Probably the most important difference between the two populations is average IQ, which undoubtedly accounts for most of the differences both in income and rates of accidental death. That the two populations should have such different incomes, yet have similar disease rates is yet more evidence that racial biology plays a crucial role in health.
Figures for individual diseases also tell an interesting story. Cirrhosis is a degenerative disease of the liver that is usually caused by drinking, and high rates are normally a sign of wide-spread alcoholism. It is not surprising that American Indians have the highest rate of cirrhosis among women and the second highest rate among men. When mothers drink heavily during pregnancy, they can give their children a form of retardation known as fetal alcohol syndrome. The number of children born with this condition for every 10,000 births is much higher in Indians than in any other group: 30. The figures for others races are blacks — 6, whites — 0.9, Hispanics — 0.8, and Asians — 0.3.
Indians also smoke more than everyone but Southeast Asians, but have the second-lowest lung cancer rates. They die from smoking-related cancers (lung, esophagus, larynx) at about half the white rate. Indians may well have a genetic resistance to lung cancer just as they have a predisposition to alcoholism.
Hispanics, many of whom are genetically related to American Indians, also seem to resist lung cancer. Although about 40 percent of Mexican-American men smoke, compared to 30 percent of white men, Mexican-Americans have about half the rate of lung cancer.
Blacks do not seem to enjoy any particular immunity. Thirty-four percent of adult blacks (as opposed to 29 percent of adult whites) smoke, and 78 percent of black smokers (as opposed to 56 percent of whites) smoke high-tar cigarettes. Blacks are also three times more likely than whites to smoke menthol cigarettes (76 percent v. 23 percent). Blacks have the highest smoking-related cancer rates of all Americans (27 percent higher than whites), and smoking is thought to account for 20 to 30 percent of all low birth weight babies in America and 10 percent of all infant deaths.
Diabetes appears to be strongly influenced by genes. The Pima tribe of American Indians has the highest rate — 50 percent — of any population in the world, and Indians in general have high rates. Blacks have even higher rates, which may be aggravated by eating habits. Every year, the average black household spends 54 percent more than the average white household on sugar. Likewise, blacks are the greatest consumers of premixed cocktails, wine coolers and other sweet drinks. Although the sugar-sweetened version of Kool-Aid claims to have 25 percent less sugar than Coca-Cola or Pepsi-Cola, blacks prefer to buy the unsweetened version and add lots of sugar.
Asians are less likely than whites to suffer from serious diseases, but there are a few exceptions. One is diabetes. Asians are more likely than whites to have the disease but less likely to die from it. Asians seem to get a less deadly or slower-acting form. Also, curiously, Asians are twice as likely as other groups to suffer from motion sickness.
Tuberculosis, though rarely fatal, is another disease from which Asians suffer at greater rates than any other group (though it would be interesting to know how much the group average is driven up by Laotians and Vietnamese). Asians are ten times more likely than whites to get tuberculosis and the figures for other groups are blacks — eight times more likely, Hispanics — five times, American Indians — 4.5 times. More than two thirds of all cases occur in the 25 percent of the population that is non-white, and nearly one third of the non-whites who get tuberculosis were born outside the United States.
There appear to be distinctly different racial susceptibilities to tuberculosis. A study of 165 racially integrated nursing homes in Arkansas found that although all patients were free of the disease when they were admitted, blacks were twice as likely as whites to become infected.
Another condition that varies by race for what are probably genetic reasons is osteoporosis. Older women who do not get enough calcium are especially prone to it, but whites suffer more than anyone else. Hip and other fractures are most common in northern European women, despite the fact that they consume more calcium than all other groups. The most likely explanations are genetically determined differences in bone accretion and bone characteristics, as well as differences in vitamin D metabolism.
Glaucoma affects blacks at five times the white rate and strikes blacks earlier. This difference is independent of socioeconomic status or access to medicine and is likely to have a genetic cause. Glaucoma is the leading cause of blindness among blacks.
Venereal diseases show starkly divergent incidence rates. Among blacks, syphilis rates per 100,000 population have soared since the introduction of crack cocaine in 1985, climbing from 50 to 140 in the five years to 1990. During the same period, the white rate declined from three to two per 100,000, which means blacks are 70 times more likely to have syphilis than whites. The 1990 figure for Hispanics is 20 per 100,000, or ten times the white rate.
Curiously, gonorrhea appears to have been unaffected by crack cocaine; from 1985 to 1990, the black rate hovered around 2,000 per 100,000 population. In 1990, that was approximately 100 times the white rate and the Hispanic rate was approximately four times the white rate. Blacks are more promiscuous than whites and less likely to take precautions against venereal disease. There appears to be no research on whether genetic reasons also account for such enormous racial differences in infection rates.
Blacks and Hispanics have higher rates of AIDS than whites, who have higher rates than Asians. Three percent of black men between the ages of 27 and 39 have the HIV virus. The figure for Hispanics is 1.7 percent and for whites it is 0.7 percent. Blacks and Hispanics — especially women — continue to contract AIDS at ever-increasing rates. Three quarters of the American women who have AIDS are non-white, as are fully 84 percent of the children who contracted it from infected parents.
r-K Theory?
With only a few exceptions, disease and death rates support the life-history theory of racial differences proposed by Prof. J. Philippe Rushton of the University of Western Ontario. To put it in far too small a nut shell, Prof. Rushton argues that of the major racial groups Asians live the longest, have the largest brains, are least preoccupied with sex, and devote the most energy to rearing small families rather than siring large ones. Whites are second to Asians, followed by blacks.
The rates at which members of different races contract and die of diseases is perfectly consistent with this pattern of what are known as r-K variables. Blacks have the highest disease and death rates, followed by whites, followed by Asians. Some races simply appear to be biologically designed to live longer than others.
Except in rare cases, it is difficult completely to isolate the biological causes of racial differences in disease rates, and some differences that seem to be biological may have unknown environmental causes. However, biological interpretations are greatly bolstered by the fact that they fit almost perfectly into the r-K pattern that Prof. Rushton has discovered. The human genome project will eventually supply the answers; in the meantime, it is a safe bet that race, not “racism,” explains most differences in disease and death rates.














