Race and Medical Care
Jason Summers, American Renaissance, October 20, 2017
I’m a registered nurse, and my career brings me in close contact with people during a very difficult time in their lives: a medical crisis. I work on a cardiac unit, which means that I’m almost always dealing with people who have had heart attacks.
Over the course of my career, I’ve noticed some distinct differences in how people of different races tend to respond to having a heart attack or to dealing with other cardiac-related problems. Some patterns are so typical of their race that before I’ve even met a patient I can often predict his race just by hearing about him from another nurse.
I deal primarily with three races: white, blacks, and Hispanics (Mestizos of Mexican origin), but I should point out that my experience is limited. I work in a very specific area of health care, and deal with a very specific kind of patient. I’ve never worked in any other nursing specialty. However, I would be very surprised if nurses in others fields didn’t experience a similar pattern of differing behaviors from race to race.
White patients
A large percentage of the patients I deal with are white. They are generally “health conscious;” they know they should be concerned about such things as eating healthfully and getting enough exercise.
Typically, when a white patient comes through my door, it’s usually someone in his fifties or sixties who just had a heart attack for the first time. The patient is shocked by the event, and wants to take steps to ensure that it doesn’t happen again. Family members are often just as shocked, and they are always filled with questions.
I experienced a typical example of this recently. A white man in his sixties had collapsed with chest pain while spending the weekend at the lake with his family. He was rushed to our hospital, and after receiving a stent in one of his coronary arteries (a process by which a blockage is repaired), he ended up in one of my rooms.
His wife showed up with him, and not much later his two adult daughters arrived. By now it was two or three in the morning, and what followed was an experience I’ve had many times with white families. After I’d gotten the patient settled into his room, I had a long conversation with the entire family about heart health. The patient wanted to know about all of the medications he would be taking — how long he’d be taking them, and what each of them did. His wife wanted to know what he should be eating, what he shouldn’t be eating. His daughter wanted to know what chance there was that he could have another heart attack.
This is all part of a clear pattern with whites: They take health issues seriously, and make plans to try to deal with them.
I’ve found that whites generally treat my expertise as a health professional with a lot of respect. They want to know what I’ve seen with other patients, and what my opinion is of their situation. They will say such things, “I know every case is different, but on average how long does it take someone to recover from this procedure?”
Black patients
The second largest patient population I deal with is blacks. In my experience, black patients and their families tend to be far less interested in their disease or its treatment. In a scenario similar to the one I described above — only with a black patient — I would not expect to spend any time answering questions about lifestyle or medications.
I began to notice early on in my nursing career that black patients care a great deal about how many snacks and drinks they can get during their stay. I remember one night, about three in the morning, helping a black patient to the bathroom. After I got him back in bed, he looked up at me and asked, “Could I get some snacks?” “Sure,” I said, “What would you like?” He answered, “Two ice creams, a can of soup, four cheese sticks, an orange juice, a grape juice, and two packs of graham crackers.”
Once, I arrived for work and received a report from the previous nurse. She began to tell me about a patient suffering from congestive heart failure, a condition in which the body retains too much fluid, resulting in difficulty breathing. “This guy has been asking for snacks all day,” she said to me. “He doesn’t want to comply with his fluid restriction and gets mad when I tell him he can’t have any more soda.” The minute I heard this, I knew that this patient was black. I even asked the nurse giving me report, “Is he black?” She gave me a shocked look, with that trace of fear that often comes into the eyes of our fellow whites when we suddenly bring up race. “How did you know?” she asked.
When I was taking care of that patient later and I asked him about his heart failure and his fluid restriction, he wasn’t interested. He did, however, complain all night about not getting enough food. He got mad at me when I told him that dining services were closed for the night, and that I couldn’t order him a second dinner. When I told him he couldn’t have any more juice drinks because he’d already reached his fluid restriction, he called in my charge nurse to complain. If heart failure patients consume more fluid than specified by their doctor, they can end up with serious respiratory problems. This patient didn’t care.
Recently I had a black female patient who had cardiac arrhythmia (an improper heart rhythm). The doctor put in a lot of orders for this patient, in particular several IV-drip medications that would be essential to treating the arrhythmia. While I was trying to get all this set up, the patient’s daughter said to me, “My mom ain’t had any dinner, she needs something to eat right now.” I replied, “We’ll take care of that later. Your mom needs this medication right now, though. I’m going to get this set up.” An hour later, when I was just starting to get the patient stabilized, the daughter again asked me, rather impatiently, “So what about mama’s supper?”
I don’t want to suggest that black patients and their families are always rude — far from it. I’ve had many pleasant and friendly black patients, and I’ve also had many rude white patients. But the racial pattern of how they think about health care is very clear. I’ve dealt with unpleasant white patients who still paid close attention to their condition and treatment, and very friendly black patients who were back for yet another treatment because they had ignored their doctor’s advice.
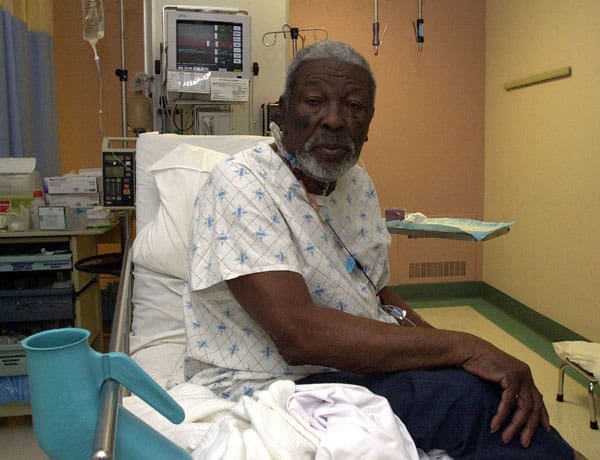
Credit Image: Toronto Star/ZUMAPRESS.com
By far the majority of my unit’s “frequent fliers” — patients who are constantly in the hospital because of a flare-up of a chronic condition — are black. Congestive heart failure is a classic problem that requires strict understanding and diligence from the patient in order to avoid recurrences.
Heart failure patients need to observe a restricted diet, which dramatically limits sodium, as well as a restriction on the amount of fluid they consume. I can’t tell you how many times I’ve checked in a black patient who simply doesn’t comply with the heart failure plan laid out by the doctor. These patients come to us very short of breath, exhausted, and weak. Often they were diagnosed with heart failure long ago, and yet when I ask them about their dietary restrictions, they simply brush the subject off, act uninterested, or claim to be compliant when it’s obvious that they are not.
These patients end up in a never-ending cycle of coming in and out of the hospital to get them out of a heart failure crisis. Hospitals go to great lengths to try to educate these patients and encourage them to stick to their plan. I’ve watched many a well-meaning, fresh-faced white nurse do her best to explain the reality of the situation to these black patients. While they are under our care, we can medicate them and control their diet, to the point that they feel pretty good. But I always know, when I discharge these patients, that I’ll probably see them again before too long, back with the same problem.
Blacks, of course, are not the only patients who can’t follow a health plan. I’ve dealt with white patients who strayed from their heart-failure regimen, but it’s much rarer, and always a very different experience. Whites tend to admit that they’ve been lax in their health plan, and to accept responsibility. Their noncompliance is usually less dramatic, so they are easier to treat.
Hispanic patients
The Hispanics I have treated are of a very specific group: Mestizos of Mexican origin. Their English is marginal or non-existent. I imagine that if I were dealing with a different Hispanic population, I might see other patterns.
My Hispanic patients are generally polite and pleasant. They are very respectful of health care staff. I use a language phone line to communicate with them, because I know that otherwise they will just pretend to understand and go along with whatever I’m saying. Even though I use a professional interpreter qualified to discuss health care matters, I still frequently doubt that the Hispanics have much understanding at all of the health and disease concepts we’re presenting to them.
Hispanics tend to show up on my unit only when a particular problem gets very bad. I’ve had many Hispanic men come days or even weeks after exhibiting cardiac symptoms. Recently I cared for a construction worker in his forties who had had chest pain for two weeks before he came to the hospital. I dealt with another Hispanic construction worker — this time in his twenties — who had a heart attack after using cocaine. He had waited three days before seeking treatment for chest pain.
I recently cared for an Hispanic woman in her fifties who came to us with weakness and shortness of breath. We discovered that she had a number of medical problems of which she was unaware, including congestive heart failure and diabetes. Even with a professional interpreter, we found it very difficult to educate her about these diseases. She was very agreeable to all the treatments and medications, but I questioned whether she really believed the doctor’s diagnosis. Her family brought several folk remedies to her, and also put some items of spiritual significance in the room. A lot of my Hispanic patients have a great deal of faith in traditional folk ideas about medical conditions.
My Hispanic patients are always surrounded by many devoted family members — something I’ve always admired — but a problem often arises when they insist on helping too much. Once I cared for an elderly Hispanic woman who was having problems getting around. We had a physical therapist working with her who insisted that she needed to be walking regularly to regain her strength. However, this patient’s family was adamant about doing everything for her. In this case, we found that the patient’s sons were literally carrying her to the restroom. I had several conversations with the family, using professional interpretation, insisting that their mother could and should begin to walk herself to the restroom.
For this woman’s family, there seemed to be a strong cultural drive to do everything for their mother. “She needs us,” her daughter told me. “We would do anything for our mama.” While I greatly respected this family’s total devotion to their elderly mother, I couldn’t help but notice how their solicitousness was slowing their mother’s recovery.
As with blacks, the great issue with Hispanic patients is long-term compliance. Even if we get Hispanic patients in optimal condition while they are with us, it is unlikely that they will go home and follow dietary guidelines, or maintain a medication regimen. Every Hispanic patient I’ve dealt with has been low-income, and we have social services at our hospital to help them can get the medication they need. The problem is getting them to work with with social services.
Conclusion
If I were to explain the problems of non-compliance I’ve had with non-whites, a leftist sociology professor would probably reply: “Well of course your approach isn’t working! You’re trying to talk to these people from a white standpoint! You’re whitesplaining!
I would agree. Modern Western medicine was created by whites. Whites are responsible for the science that makes our health care possible, and whites built the elaborate American medical system we enjoy. Health care workers are trained with the assumption that they’ll be working with patients who will cooperate in planning out a health plan for them, and will change their habits to accommodate that plan. Overwhelmingly, this is how white patients behave; non-whites often do not.
None of this is surprising. Whites evolved in harsh climates that required long-term planning. Blacks evolved in warmer climates that made them more present oriented. It’s strange to live in a society that simply will not acknowledge basic realities.
I’ve often imagined what it would be like to practice health care in a white nation. It would be far more efficient and effective because we would be treating the kind of patients who share the values and expectations of the creators of our modern medical system.
Perhaps it’s time that we started listening to leftist sociologists. Perhaps we should strop whitesplaining health care to non-whites. Perhaps we should let non-whites have their own approach, while we provide health care for our people in our own way.
If you have a story about how you became racially aware, we’d like to hear it. If it is well written and compelling, we will publish it. Use a pen name, stay under 1,200 words, and send it to us here.














